The thoracic duct is more like a vein histologically with the primary function of transporting chyle from the gastrointestinal tract into a systemic venous system. It carries almost 4 liters of chyle daily, most of which originates in the digestive tract. The flow rate can be up to 100 ml/kg/day, depending on the diet consumed. A combination of intrathoracic and intraabdominal pressures and arterial pulsations helps in maintaining lymph flow in the thoracic duct. Chyle is rich in chylomicrons, triglycerides, cholesterol, fat-soluble vitamins and also contains albumin in high concentrations (12-14 g/L). Thoracic lymph also contains lymphocytes, which account for 95% of the cell content, and this keeps chyle mostly sterile. Electrolytes and other enzymes levels resemble that of the plasma [10,11].
Conservative therapy is typically used initially but if there is an active chylous drainage from the wound, exploration and ligation of ductus is appropriate treatment. But, if the diagnosis is made only with a chylothorax, treatment should be attempted conservatively by drainage and early total parenteral nutrition initially. If spontaneous closure of the duct does not occur within 14 days, the decision of definitive surgery should be taken. Empirically, it is generally agreed that surgical correction of the fistula should be considered before the patient becomes severely malnourished. Presence of 1,000–1,500 ml/day of drainage for 5 days or 500 ml/day of chylous drainage for 14 days despite medical treatment necessitates surgical intervention [12,13].
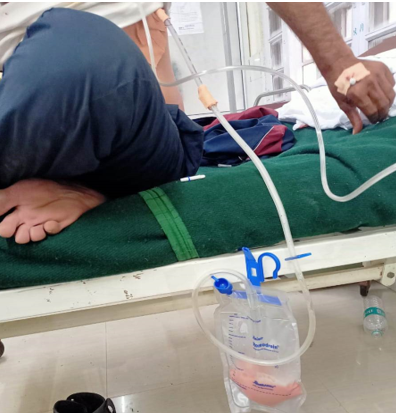
Possible side effects after chylothorax depend on the size of the leakage, duration and mode of treatment applied. There may be cardiopulmonary problems, metabolic and immunological deficits due to loss of proteins, lipids and lipid-soluble vitamins [12,14]. The most common disturbances described are hypovolemia, hyponatremia, hypoproteinemia and hypocalcemia [14]. Thus, the intake and output of the patient and biochemical parameters should be monitored during nutritional support, and replacements should be provided accordingly. About half of chylothorax cases can be treated by conservative measures. [12,13]. Initially, a tube tracheostomy should be applied for decompression and drainage. Chylous drainage increases the electrolyte loss and nutritional requirements. Thus, adequate and sufficient nutrition should be provided. If the patient receives oral nutrition, lipid intake should be limited to 20–30 g/day and medium-chained triglycerides, which pass into the portal system without joining the lymphatic system, should be used. [13] Closed chest drainage prevents the accumulation of chyle in the pleural cavity and facilitates the monitoring of chyle output, whereas hyperalimentation and bowel rest significantly reduce chyle production [12]. Chyle formation is closely correlated with enteral fat. Most conservative regimens involve a low-fat diet supplemented with medium chain triglycerides to reduce chyle production. But it must be remembered that any oral feeding will increase the output of the chyle fistula. Therefore, complete gut rest and TPN appear to provide the best conditions for fistula closure and nutritional support when available. [15] When TPN is started early it helps to maintain rather stable and metabolically balanced condition. The duration of the trial of conservative management has not been so far uniformly stated.