An epidermal inclusion cyst is the most common cutaneous cyst. Epidermal inclusion cysts are also known as epidermal cysts, epidermoid cysts, infundibular cysts and keratin cysts.Epidermal inclusion cysts are sometimes referred to as “sebaceous cysts,” however this is a misnomer as this lesion does not involve the sebaceous gland. The term “sebaceous cyst” should only be used in association with steatocystoma multiplex [2,3].
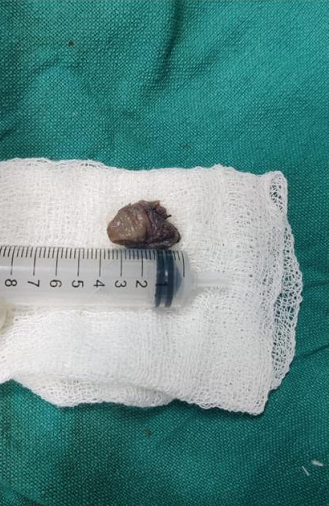
An epidermal inclusion cyst typically appears as a slowly enlarging, mobile, dome-shaped lump, filled with keratin material and located just below the surface of the skin. They can range in size from 0.5 cm to several centimeters. Often times, there is a “punctum,” or small dark-colored opening on the surface of the epidermal inclusion cyst, which connects to the cyst located below skin’s surface. Through the opening, the keratin material may be drained out.Epidermal inclusion cysts are generally considered benign (non-cancerous), although there have been rare cases of malignancy arising within the cyst[2-4].
Epidermal inclusion cysts are the most common type of skin cyst. They can be located anywhere, but are most common on the face, followed by the chest or back, scalp, neck, legs, arms and/or genitalia.Epidermal inclusion cysts are often asymptomatic. However as the keratin accumulates within the cyst, the cyst may increase in size, become sore or painful, and eventually rupture, leading to the drainage a foul-smelling, white to yellow “cheese-like” material [3-5].
Epidermal inclusion cysts are common and typically harmless, but rarely can become malignant (cancerous). Approximately 1% have been shown to transform into malignancy.An epidermal inclusion cyst may concerning if it has Signs of infection, including pain, redness, swelling and/or drainage, A fast rate of growth and a diameter larger than five centimeters [4,5].
Although they can appear at any age, epidermal inclusion cysts most frequently occur during early to mid-adulthood (ages 20-60s). Epidermal inclusion cysts rarely appear before puberty. They are one and a half times more common in males than in females.An epidermal inclusion cyst does not typically go away by itself completely unless removed surgically, by an excision. However, an epidermal inclusion cyst may shrink in size and stay asymptomatic for quite some time, and no treatment may be necessary.Most epidermal inclusion cysts occur at random [3,4].
Some genetic conditions may be associated with the development of multiple epidermal inclusion cysts like Gardner Syndrome (Familial Colorectal Polyposis), Gorlin Syndrome (Basal Cell Nevus Syndrome) and Favre-Racouchot syndrome [1,2].
Epidermal inclusion cysts are formed from the follicular infundibulum, which is part of the hair follicle. Epidermal inclusion cysts form when the follicular infundibulum is disrupted, or when the surface of the skin becomes implanted below the skin through an injury or trauma in the area, such as a scratch, surgical wound or a skin condition like acne [2,4].
The main symptom of an epidermal inclusion cyst is a small moveable lump under the skin. The lump is usually not painful. In some cases, however, cysts can get inflamed and become tender to the touch. The skin on the area of the cyst may be red and/or warm. Usually, healthcare provider can diagnose an epidermal inclusion cyst with a simple examination of the skin. In some cases, the healthcare provider will perform a biopsy to rule out other skin growths [2,3].
If healthcare provider suspects that your epidermal inclusion cyst is, he or she may order, the tests including an ultrasound may help determine the contents of the cyst, A punch biopsy. This is where a small amount of the tissue from the cyst is removed and examined for signs of cancer. A CT scan may be helpful in confirming the diagnosis of a large epidermal inclusion cyst and help the surgeon determine the best plan for removal [4,5].
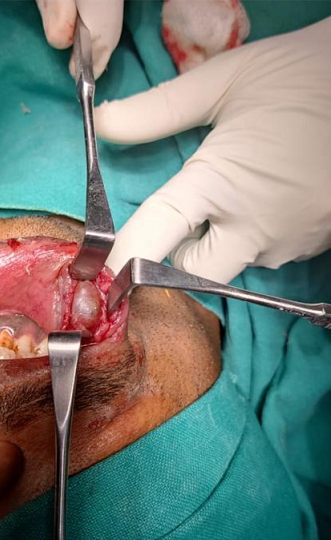
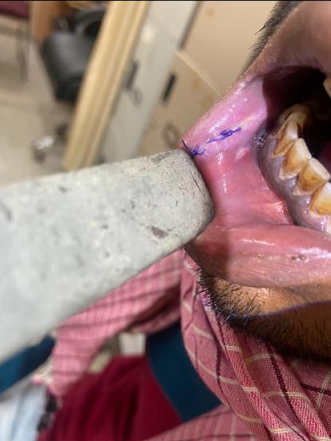
In many cases, epidermal inclusion cysts can be left untreated and monitored, as they are not dangerous, and especially if they are not causing any symptoms.If a cyst becomes inflamed or painful, your healthcare provider may consider treating the epidermal inclusion cyst with Injection of steroid medication - to reduce swelling, which may help temporarily. Surgical excision - The cyst is usually removed using an injection of local anesthetic to numb your skin. This procedure will leave a small line scar after the cyst is removed.Risks of surgical excision of a cyst include a small chance of bleeding, infection and likely a small scar over the area where the cyst is removed [3,4].