The median age of diagnosis of rectal cancer is 63 years for both men and women [5]. Moreover, only 3% of rectal cancer presents with single metastasis to the nervous system as compared to single metastasis to the liver (62%) or thorax (19%) [6]. Incidence of a brain metastasis from colorectal cancer is relatively rare with an incidence of approximately 0.6 to 3.2% [6]. Brain metastasis is much more common with ca lung, ca breast, testicular cancer and melanoma with an incidence ranging from 10-50% depending on the type of cancer [6].
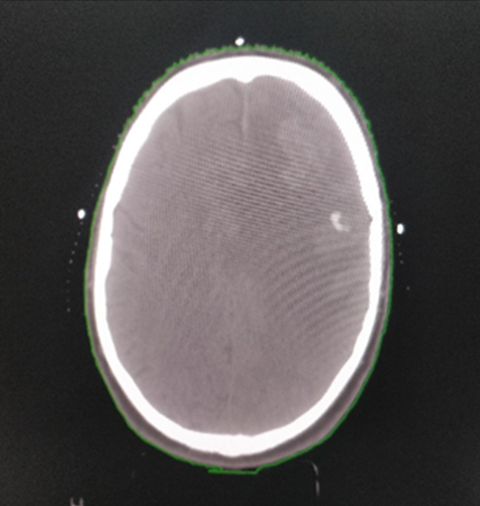
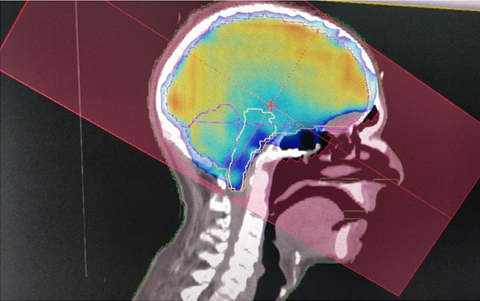
MRI imaging of the brain in patients with colorectal cancer having any neurological symptoms or risk factors for brain metastases such as the presence of lung metastases, KRAS mutation, high Carcinoembryonic Antigen (CEA) level, or rectal cancer is highly recommended [7].
A recent metanalyses expresses the concern of microsatellite instability leading to proximal colon cancer with RAS and BRAF mutations found in approximately 52% [8] and 10% [9] of colorectal cancer, respectively. However, our patient did not have any evidence of microsatellite instability or a proximal colon cancer, still RAS and BRAF mutation testing has been shown to have prognostic and predictive value in metastatic colorectal cancer. Treatment with Anti-Epidermal Growth Factor Receptor (EGFR) antibodies has been shown to be less effective in patients with KRAS mutations [10] and patients with metastatic colorectal cancer. Patients with KRAS or BRAF mutations have been shown to have worsened outcomes [11].