A 56-year-old female patient reported to us complaining of:
Multiple joint pains for 5 years
Along with that patient also complained of dryness of mouth, for 1 year, and dryness of eyes for 4-5 years
Extra oral examination showed bilateral parotid gland enlargement present on the right and left side of the parotid region.
On an inspection swelling on right and left of the parotid gland, measuring about 2.8 cm × 2.4 cm in diameter. On palpation it was diffuse, firm, non-movable, warm, tender on palpation, overlying surface texture was normal, along with that dryness of eyes, fever was also noted. Bilateral submandibular lymph nodes were palpable. Intra-oral examination shows dry tongue.
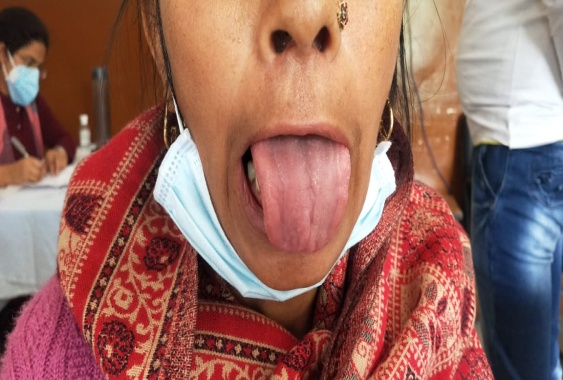
Figure 1: Complete Hemogram
Complete hemogram showed increased erythrocyte sedimentation rate. Schirmer test was less than 5mm (Figure 1). ANA, RA Factor, Anti- ccp, Anti SSa was positive. RA factor was positive for rheumatoid arthritis. Ultrasonography shows bilateral submandibular and parotid gland enlargement with multiple hypoechoic lesions within showing very high vascularity, likely to present systemic disorder like Sjögren’s syndrome. Incisional biopsy of lower lip was not done as patient was not giving consent.
Based on history, clinical presentation of the patient, and above investigatory findings, a confirmatory diagnosis of Secondary Sjögren syndrome was made with underlying disease being rheumatoid arthritis.



